Diabetic retinopathy is an eye disease that affects the retina found in patients with diabetes. It is a leading cause of blindness in American adults. Chemical changes caused by diabetes can damage blood vessels throughout the body, including the fine blood vessels in the retina, or the seeing part of the eye. This damage is called diabetic retinopathy.
There Are Two Kinds of Diabetic Retinopathy:
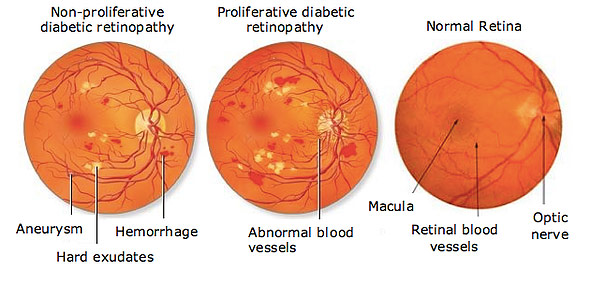
Nonproliferative Diabetic Retinopathy (NPDR)
NDPR occurs when the retinal blood vessels start to leak, causing blood or fluid to seep into the retina. The retina becomes thick and swollen and does not work correctly. If the leaking happens in the macula, (the central part of the retina), vision will be blurred. If the leaks occur in the periphery of the retina, there may be no impact to vision.
Proliferative Diabetic Retinopathy (PDR)
PDR occurs when the retinal blood vessels close, cutting off nutrition to the retinal tissue. Abnormal new blood vessels, called neovascularization, may form as the body’s response to the damaged native vessels. These abnormal blood vessels can cause bleeding inside the eye (vitreous hemorrhage), they can cause the pressure in the eye to rise to a dangerous level (neovascular glaucoma) and they can cause scar tissue that detaches the retina (tractional retinal detachment). Scar tissue, high eye pressure or lack of blood-flow can result in blindness if not treated. The earlier neovascularization is discovered (and treated), the better the chance that surgery can preserve vision. Both types of diabetic retinopathy may occur without a noticeable change in vision at first. It is therefore imperative, if you have diabetes, to have your retinas examined by an eye specialist (see prevention below).
In 2012, diabetes affected 29 million Americans and is the leading cause of new cases of blindness in people age 20 to 74. There are almost 8 million Americans with diabetic retinopathy and that number is expected to reach 14 million by the year 2050. Each year thousands of people will lose their sight from this disease. Vigilant care, however, can markedly reduce the risk of visual complications from diabetes. And for those that do develop problems, new treatment technology offers hope for saving or recovering some sight.
What Is Diabetes?
Diabetes is a chronic disease in which the body does not produce or properly use insulin, a hormone that helps convert sugar and food into energy. The biochemical reactions that occur because the body doesn’t have the proper amounts of blood sugar can have a profound impact on the eyes. Diabetes can cause changes in the lens in the eye that leads to early cataract, contribute to dry eyes, damage the innervation of the eye and also cause damage to the blood vessels that nourish the retina. The constant thickening and thinning of the natural lens due to dramatic swings in blood sugar levels leads to blurry vision early in the disease. For people who are unaware that they have diabetes, blurry vision is often the first signal that something is wrong.
Prevention of Eye Disease for the Diabetic
- Blurry vision is a warning to get blood sugar levels under control under the direction of a primary care doctor or endocrinologist. This can be achieved through a combination of diet, exercise and medication.
- Keeping good track of your diabetes disease involves monitoring your blood sugar and knowing your glycosylated hemoglobin, or hemoglobin A1C test. The A1C test is a measure of your average blood sugar for the previous 3 month period. For most people, the goal is to keep the A1C level below 7.0 to prevent both eye and health complications from diabetes.
- Keep your blood pressure and cholesterol under control.
- Ask your doctor for help quitting tobacco products.
- Get your eyes checked regularly. Patients with a new diagnosis of diabetes mellitus type II (most people with diabetes) should have a dilated exam soon (within a month or two) after diagnosis, as eye damage could be starting without any symptoms of blurry vision. Younger patients with a new diagnosis of diabetes mellitus type I should have a dilated eye exam within 5 years of diagnosis, unless they have symptoms of blurry vision sooner.
Those diabetic patients who already have diabetic retinopathy should follow the prevention recommendations above (blood sugar, blood pressure, cholesterol control and avoidance of tobacco products) to lower the chance of losing vision from diabetes. Diabetic retinopathy can sometimes progress despite improvement in health and should be followed closely by a retina specialist to ensure the best prognosis.
What Testing is Done to Evaluate Eye Disease in Diabetics?
A thorough exam is done by your doctor which involves checking your vision, eye pressure, eye motility, optic nerve function and peripheral vision. Exams are done by dilating the pupils to thoroughly assess any abnormalities in the back of the eye (retina). Your doctor is looking for any signs of swelling in the retina, bleeding, abnormal growth of blood vessels, retinal detachment and glaucoma associated with diabetes. In addition, special testing is done on site which include:
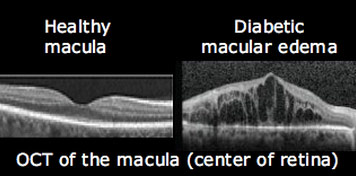
- Optical coherence tomography (OCT)
- Fluorescein angiography (FA)
How is Diabetic Retinopathy Treated?
For patients with non-proliferative diabetic retinopathy (NPDR) with swelling in the macula (diabetic macular edema), there are several treatment choices:
Intravitreal injections of anti-vascular endothelial growth factor (anti-VEGF) medicines:
This treatment involves delivering medicine directly into the inside of the eye to chemically bind the signals that causes leaking into the eye.
For Spanish version, click here ›
New treatment options:
In addition to the treatments discussed above, we anticipate that within the next 5-10 years, there will be additional treatment options available that will potentially be more effective, less invasive, and more durable. New England Retina Associates is actively involved in clinical trials to help identify the most effective treatments for diabetic retinopathy.
For Further Information
- American Diabetes Association
- National Eye Institute: Diabetic Eye Disease
- AAO: What Is Diabetic Retinopathy?
